Document Type : Original Research Article
Authors
- Munawaroh Fitriah 1
- Cynthia Ayu Permatasari 2
- Jusak Nugraha 1
- Betty Agustina Tambunan 1
- Hartono Kahar 1
- Aryati Aryati 1
1 Department of Clinical Pathology, Faculty of Medicine, Universitas Airlangga /Dr. Soetomo General Academic Hospital, Surabaya, Indonesia
2 Clinical Pathology Specialization Program, Faculty of Medicine, Universitas Airlangga, Surabaya, Indonesia
Abstract
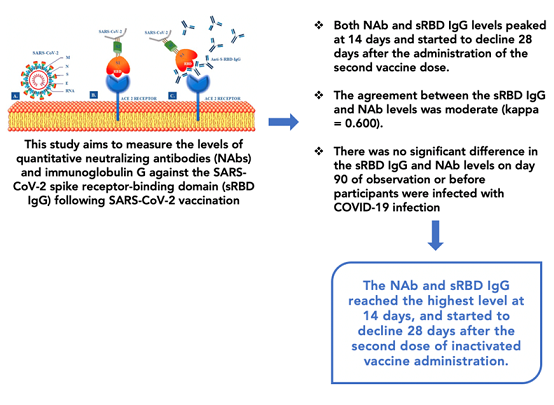
The primary objective of this study is to assess the quantifiable neutralizing antibody (NAb) levels and the concentration of immunoglobulin G against the spike receptor-binding domain (sRBD IgG) of the SARS-CoV-2 virus post-vaccination. This observational research was carried out within the premises of Dr. Soetomo Hospital, situated in Surabaya, Indonesia, and targeted healthcare professionals. A cohort of 50 healthcare workers was selected for participation. Blood specimens were gathered on five separate occasions from each participant. The initial sample was procured before the initial dose of the CoronaVac inactivated vaccine was administered, while the subsequent samples were taken at intervals of 14, 28, 90, and 180 days after the second dose. Quantitative evaluations of NAb and sRBD IgG levels were executed employing a chemiluminescent immunoassay using the Autobio AutoLumo A1000 analyser. The zenith of both NAb and sRBD IgG levels occurred at the 14-day mark, subsequently displaying a decline after 28 days post the second vaccine administration. The concordance between sRBD IgG and NAb levels exhibited a moderate correlation (kappa = 0.600). No statistically noteworthy disparity was detected in sRBD IgG and NAb levels by the 90th day of observation or before participants encountered instances of COVID-19 infection. The peak concentrations of NAb and sRBD IgG were attained at the 14-day milestone yet experienced a descent commencing 28 days after the second inactivated vaccine dose administration.
Graphical Abstract
Keywords
Main Subjects
Introduction
The global impact of the SARS-CoV-2 virus, leading to the COVID-19 pandemic, has resulted in extensive fatalities and far-reaching societal and economic challenges. Measures such as social distancing, ubiquitous mask usage, improved hand hygiene, and prompt isolation of infected individuals have contributed to curtailing viral transmission within communities. The availability of SARS-CoV-2 vaccines by the close of 2020 played a pivotal role in significantly reducing infection rates [1,2]. Regulatory bodies, including the Food and Drug Administration (FDA), authorized the emergency use of mRNA-based, recombinant, and inactivated vaccines, including CoronaVac, Sinopharm, and Covaxin. On June 1, 2021, the World Health Organization (WHO) granted emergency validation for the CoronaVac vaccine. By March 17, 2022, over two billion doses of CoronaVac had been administered across 52 countries [3,4]. However, the question remained whether all individuals mounted an antibody response, with a 5% susceptibility to breakthrough infections, or if a modest proportion of individuals remained non-responsive, staying at risk for infection [5].
Coronavirus infections typically trigger the production of neutralizing antibodies (NAbs). These NAbs, generated by B lymphocytes, can hinder viral infection at various stages of the virus replication cycle, particularly during viral binding and entry into host cells. NAbs can facilitate viral particle aggregation, reduce the number of virions attaching to host cells, impede virus internalization through endocytosis, degrade the virus, or thwart viral replication and transcription processes. The pivotal role of NAbs is their ability to obstruct infection by interfering with the virus's receptor-binding domain (RBD) during the virus-cell attachment process [6,7].
The plaque reduction neutralization test (PRNT) stands as the benchmark method for gauging NAb levels, yet its feasibility for large-scale serodiagnosis and vaccine assessment is limited [6,8]. Establishing baseline measurements and post-vaccination tracking of anti-SARS-CoV-2 NAbs and immunoglobulins (Igs), specifically targeting and incapacitating the spike protein and/or its RBD, has emerged as a cornerstone for monitoring vaccine effectiveness and the persistence of humoral immune responses [9]. Different antibody assay platforms exhibit variations in the detected antibody isotypes, while the chief challenge in appraising immune protection against SARS-CoV-2 infection lies in the absence of consensus regarding a precise, high-capacity testing approach [10]. The evaluation of commercially available surrogate NAbs becomes particularly significant, especially for settings with limited resources to conduct PRNT assays. In this context, we present findings on a novel commercial chemiluminescent immunoassay (CLIA) aimed at assessing the durability of IgG directed against the spike RBD (sRBD IgG) and quantifying NAb levels post-vaccination.
Materials and methods
Study design and setting
This study was designed as a forward-looking observational cohort investigation carried out at Dr. Soetomo General Academic Hospital.
Participants and variables
All participants provided their informed consent through signed documents, and the study was granted approval by the health research ethics committee of RSUD Dr. Soetomo (Approval No. 0141/KEPK/II/2021). Eligible participants were healthcare workers aged 18 to 59 years, designated for CoronaVac vaccination, capable of receiving the complete two-dose regimen, committed to adhering to the study's timeline, and who formally consented to participation.
Exclusion criteria encompassed individuals with a documented history of SARS-CoV-2 infection prior to vaccination. The study enrolled a total of 50 healthcare workers who received both doses of the CoronaVac vaccine between January and March 2021.
The vaccination protocol consisted of a duo of CoronaVac doses, spaced four weeks apart. Venous blood samples were procured prior to the initial vaccination (designated as day 0), as well as at intervals of 14, 28, 90, and 180 days subsequent to the second CoronaVac dose (with a permissible variance of ±1 day).
Laboratory measurements
Blood samples were extracted through venipuncture and stored in serum separator tubes containing clot activator and gel. The serum was subsequently partitioned into discrete aliquots and cryopreserved at -70 °C until analysis. The assessment of quantitative anti-SARS-CoV-2 neutralizing antibodies (NAb) and spike receptor-binding domain (sRBD) immunoglobulin G (IgG) responses was conducted utilizing SARS-CoV-2 NAb Q and anti-SARS-CoV-2 RBD tests, employing the Autobio AutoLumo A1000 chemiluminescent immunoassay platform (Autobio Diagnostics, China). The NAb and sRBD IgG levels in the Autobio assays were expressed as international units per milliliter (IU/mL) and arbitrary units per milliliter (AU/mL), respectively. The established cutoff values for positive results were >30 IU/mL for SARS-CoV-2 NAb Q and >8 AU/mL for anti-SARS-CoV-2 RBD. All tests were executed in alignment with the manufacturer's protocols.
Statistical analysis
Variations in SARS-CoV-2 antibody levels across different observation days were subjected to analysis utilizing the Friedman test, followed by the Wilcoxon signed-rank test. Visual representation of antibody kinetics was provided through diagrams. In addition, kappa statistics were used to verify the agreement between the quantitative NAb and sRBD IgG levels. Disparities in antibody responses within the subset of participants with and without SARS-CoV-2 infection during months 3 and 6 of observation, as well as differences according to comorbidities, were examined using the Mann–Whitney test.
Results
Participants
Table 1 presents the demographic details of the participants. A cohort of 120 healthcare workers was initially enlisted, with 50 individuals successfully tracked throughout the complete 6-month study duration. Among these, 31 participants were identified as female, and the mean age was recorded at 35.74 ± 6.99 years. In addition, 23 participants had comorbidities, mainly hypercholesterolemia and hypertension. Notably, a subset of 10 participants was confirmed to have contracted SARS-CoV-2 infection between months 3 and 6 of observation. The median duration from the second vaccine dose to infection onset was calculated at 151 days (interquartile range: 144–164 days).
Antibody measurements
The quantitative NAb and sRBD IgG levels of all participants are shown in Table 2, while the antibody kinetics is shown in Figure 1. Both NAb Q and sRBD IgG levels reached their zenith at the 14-day mark and subsequently exhibited a decline by the 28-day interval following the second dose vaccine administration. The quantitative NAb and sRBD IgG levels changed between the days of observation and significantly differed before and after vaccination (p<0.001; Table 2). In addition, the differences between the days of observation were continuously analysed using the Wilcoxon signed-rank test, consistently yielded statistically significant outcomes (p<0.001; Table 3).
Discrepancies in NAb and sRBD IgG Levels Pre- and Post-Vaccination within the Entire Cohort (n = 50) were assessed using the Wilcoxon signed-rank test. Results indicated non-significant distinctions between day 180 and days -14, -28, -90 regarding NAb (p = 0.102, 0.188, and 0.347, respectively). Similarly, no significant differences were observed between day 180 and days -28, -90 for sRBD IgG (p = 0.188, 0.347).
The agreement between the sRBD IgG and NAb Q levels was also analysed. There was high agreement between the median sRBD IgG and NAb Q levels on days-14 (r = 0.600; p < 0.00), -28 (r = 0.600; p < 0.00), and -180 post-vaccination (r = 0.600; p < 0.00).
Analysis of comorbidities
The participants without COVID-19 were further classified according to the presence of comorbidities to determine whether comorbidities affect the NAb Q and sRBD IgG levels. The NAb Q and sRBD IgG levels were significantly lower in the 6th month in the participants with comorbidities (p < 0.05; Table 3).
Discussion
The evaluation of baseline individual anti-SARS-CoV-2 neutralizing antibody (NAb) status and the subsequent monitoring of humoral immune responses post-vaccination play pivotal roles in combatting COVID-19 [9,11-12]. A comprehensive understanding of seroprevalence rates and the kinetics of humoral immune responses is fundamental for devising effective vaccination strategies [13,14].
Given the gradual waning of humoral anti-SARS-CoV-2 immunity over time, and the reliance on commercial immunoassays to gauge this response, personalized insights can be gleaned [9,15,16]. Evidently, the general trends of immune responses are akin across vaccine recipients, manifesting as a surge in SARS-CoV-2 S1 IgG production within 1-2 weeks after the second dose, followed by a gradual attenuation in antibody levels [5]. Our findings corroborate that both spike receptor-binding domain (sRBD) IgG and quantitative NAb levels initiated their descent by the 28-day mark post the second vaccine administration, mirroring earlier observations pertaining to antibody kinetics associated with inactivated vaccines [17-20]. Analogously, a decline in vaccine-triggered neutralization titers within the initial 6 months post the second vaccine dose administration has been documented across various vaccines [21-23]. This prompts contemplation regarding the potential implementation of supplementary vaccine boosters as SARS-CoV-2 antibody titers diminish.
Commercial serological assays targeting SARS-CoV-2 antibodies, although available, necessitate comprehensive assessment. Among the structural proteins of the coronavirus, the spike (S) and nucleocapsid (N) proteins hold the principal immunogenic roles [24]. The S protein is comprised of two subunits: S1, housing the receptor-binding domain (RBD), and S2 [25-27]. Our previous findings indicated that the median sRBD IgG level on day 28 significantly exceeded the NAb level [18]. However, in the current study, we observed a moderate level of concordance between sRBD IgG and quantitative NAb levels 14 and 28 days following the second vaccine dose administration. Divergence in these observations could be attributed to the utilization of distinct assays for evaluating sRBD IgG and NAb levels. A prior investigation juxtaposed five commercial chemiluminescent immunoassays (CLIAs) for detecting anti-SARS-CoV-2 total antibodies and IgG; while overall compatibility was evident, disparities could arise based on the target antigen and the vaccine type [9]. The agreement between assays on day 90 demonstrated less consistency. The measured NAb levels encompassed not only IgG but also IgE and IgM levels. Despite variations in the literature concerning IgM and IgG kinetics, a prevailing consensus suggests that IgM, IgA, and IgG responses are evoked 1-2 weeks following symptom onset in the majority of SARS-CoV-2 cases. IgM levels dwindle rapidly around day 20 and become undetectable by day 60 post-onset [28-30]. In comparison, IgA levels exhibit a gradual decline, persisting at a lower level than IgG. The transition from SARS-CoV-2 IgM to IgG is swift, transpiring within 7 to 14 days. Notably, the attenuation of IgG production transpires at a significantly slower pace than that of IgM, with antibody persistence generally spanning 3-5 months [18,28]. Furthermore, SARS-CoV-2-specific IgG may endure for up to 8 months [31]. Further investigations have unveiled the potential for the detection of SARS-CoV-2-specific IgG even a year post-infection [14,32-33].
Within the confines of this study, a subset of 10 participants succumbed to confirmed COVID-19 post the third month of observation. The occurrences of infection in these individuals coincided with the emergence of the second wave of cases in Indonesia, predominantly propagated by the novel SARS-CoV-2 variant- the delta variant. Strikingly, breakthrough infections were observed even among individuals who had received complete vaccination. Notably, the occurrence of breakthrough infections among fully vaccinated healthcare workers was found to be correlated with neutralizing antibody (NAb) titers during the peri-infection period [34]. Interestingly, our study yielded no significant distinctions in the kinetic trajectories of quantitative NAbs and sRBD IgG on days 14, 28, and 90 (prior to infection) between participants with and without COVID-19. This intriguing revelation suggests that there exists no notable dissimilarity in the humoral immune response between the two participant groups. The risk associated with acquiring COVID-19 is believed to be influenced by factors such as declining antibody levels, the presence of distinct SARS-CoV-2 variants, disparities in individual immune reactions, and variances in exposure levels [35]. Moreover, beyond merely reducing transmission rates, vaccination is anticipated to curtail disease severity. It has been observed that vaccinated individuals who encounter breakthrough infections, including those involving the delta variant, are less prone to developing symptomatic manifestations, exhibit accelerated recovery, and manifest a significantly diminished likelihood of requiring hospitalization when compared to their unvaccinated counterparts- findings that align harmoniously with our study results [14,36].
The NAb Q and sRBD IgG levels were significantly lower in the 6th month following vaccination in the participants with comorbidities than in those without comorbidities (p<0.05). It is widely observed that individuals bearing comorbidities often manifest attenuated immunological reactions to infections or vaccinations, consequently warranting potential considerations for increased vaccine dosages or an earlier introduction of supplementary booster vaccines [37-41].
This investigation was confined to a solitary institution, focusing exclusively on the humoral immune response to vaccination based on the vaccine’s ability to induce sRBD IgG and NAb production without determining the correlation of the results with those of the PRNT. While antibodies serve as a fundamental gauge of vaccine effectiveness, the role of memory B and T cells in conferring enduring protection introduces another dimension to this study's limitations. In addition, a larger number of participants, various types of vaccines, and booster effects need to be further evaluated.
Conclusion
Both sRBD IgG and NAb Q levels were evaluated using a chemiluminescence-based method (Autobio AutoLumo 1000), which showed moderate agreement. The kinetics of sRBD IgG and NAbs peaked at 14 days and declined to begin 28 days post-administration of the second dose of the inactivated vaccine, underscoring the potential requirement for booster interventions. There was no difference in the sRBD IgG and NAb Q levels on day 90 between the infected and uninfected participants during the 90- and 180-day observation. Antibody levels might not be the only factor contributing to the prevention of COVID-19; hence, sustained preventive measures against SARS-CoV-2 infection remain imperative.
Acknowledgments
Our heartfelt appreciation extends to the dedicated clinical pathology research laboratory personnel who facilitated the storage and examination of the samples.
Funding
The authors disclosed receipt of the following financial support for the research, authorship, and/or publication of this article. The reagents used in this study was provided by the Autobio AutoLumo A1000 team (PT. Gracia Visi Pratama).
Authors' Contributions
MUF: Analysing data and write the manuscript. CAP: recruiting subject, informed consent and collect the specimen for the examination. JUN and HAR: Consultation for the testing, also revise the manuscript. BAT and ARY: recruiting subject, analysing data of the testing and revise the manuscript.
Conflict of Interest
All authors affirm the absence of any conflicting interests.
Orcid:
Munawaroh Fitriah: https://orcid.org/0000-0002-7617-9874
Cynthia Ayu Permatasari: https://orcid.org/0000-0002-9375-8982
Jusak Nugraha: https://orcid.org/0000-0001-6700-9921
Betty Agustina Tambunan: https://orcid.org/0000-0002-3214-993X
Hartono Kahar: https://orcid.org/0000-0002-1379-5004
Aryati Aryati*: https://orcid.org/0000-0002-9383-6354
-------------------------------------------------------------------------------
How to cite this article: Munawaroh Fitriah, Cynthia Ayu Permatasari, Jusak Nugraha, Betty Agustina Tambunan, Hartono Kahar, Aryati, Quantitative neutralizing antibody using chemiluminescence assay for evaluating antibody response following inoculation of inactivated vaccine among healthcare workers in Surabaya, Indonesia. Journal of Medicinal and Pharmaceutical Chemistry Research, 2024, 6(8), 1130-1141. Link: https://jmpcr.samipubco.com/article_193193.html
-------------------------------------------------------------------------------
Copyright © 2024 by SPC (Sami Publishing Company) + is an open access article distributed under the Creative Commons Attribution License(CC BY) license (https://creativecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.

.png)
.png)
.png)
.png)
.png)
.png)
