Document Type : Original Research Article
Authors
Department of Child Health, Dr. Soetomo General Academic Hospital, Universitas Airlangga, Surabaya, Indonesia
Abstract
Biliary atresia (BA) is a progressive inflammatory and non-obstructive disorder with unclear etiology. BA management has yet to obtain satisfactory results. The pathogenesis is currently unclear, thought to have originated from bile duct epithelium viral infection, followed by an Epithelial-Mesenchymal Transition (EMT) process that ended with biliary cirrhosis. This study aimed to examine the changes of E-cadherin and N-cadherin expressions in mice model biliary atresia. Forty-eight newborn mice (Balb/c) were randomized into two groups that received a placebo and 1.5 x106 plaque-forming units (pfu) of rhesus rotavirus (RRV) intraperitoneally within less than 24 hours after birth. Each group was terminated on days 3, 7, 14, and 21, further examining the expressions of E-cadherin and N-cadherin with flow cytometry. Statistical analysis was done using Mann-Whitney and Kruskal-Wallis. The mean initial weight of the newborn was 1.82 grams (heterogeneity p = 0.2). A total of 48 samples were found in the study. However, only 39 were able to be included (9 newborn mice were dead). There were differences in the expressions of E-cadherin and N-cadherin (p=0.01). Interaction expression between days and group differed significantly with p<0.001. Cadherin Switch or ratio expressions between E-cadherin and N-cadherin with p<0.001. Induction and duration of illness after RRV exposure influence the expressions of E-cadherin, N-cadherin, and cadherin switch in the murine model of biliary atresia.
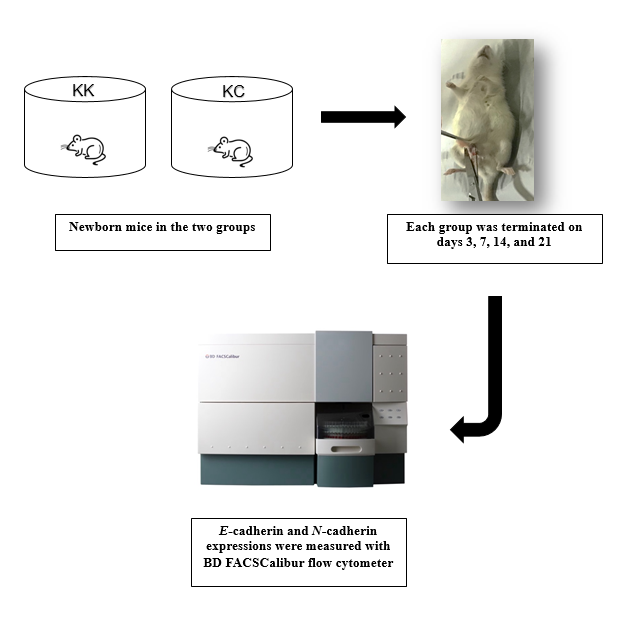
Graphical Abstract
Keywords
Main Subjects
Introduction
Biliary Atresia (BA) is a progressive inflammatory obstruction and fibro-obliteration of part or total of extrahepatic and intrahepatic bile ducts during the perinatal period [1-3]. Biliary atresia occurs in about 1 in 8,000 to 18,000 live births, and 50-60% require liver transplantation [4,5]. Additional evidence indicates that the documented incidence rate of biliary atresia in the Asian and Pacific Islander populations is 1 in 5500. There is currently a lack of public official statistics regarding the occurrence of BA in Indonesia [5,6].
The cause of AB is still unclear. Several factors are suspected to play a role in the pathogenesis of biliary atresia AB, including infection, fetal circulatory disturbance, morphogenesis abnormalities, exposure to toxins, and immunologic abnormalities. Perinatal hepatobiliary viral infections will cause apoptosis or chronic necrosis of cholangiocytes [7,8]. Infections by viruses such as Reoviridae (Reovirus and Rotavirus) with a double-stranded RNA (dsRNA) are suspected. However, contradictory results have also been reported [9].
Bile duct epithelial cells allegedly change in characteristics of epithelial cells into mesenchymal cell characteristics due to cell polarity loss, intercellular communication, and loss of normal epithelial cell structure accompanied by extracellular matrix accumulation MES [10,12]. This process is known as Epithelial-Mesenchymal Transition (EMT) [13,14].
Several hepatobiliary disorders, including BA, have been linked to periductal and portal fibrosis through the epithelial-mesenchymal transition (EMT) of biliary epithelial cells (BECs) [9].
Loss of intercellular adhesion molecules (E-cadherin and occludins), down-regulation of epithelial markers (cytokeratins), up-regulation of mesenchymal markers (vimentin and smooth muscle actin), and acquisition of a fibroblast-like (spindle) morphology with cytoskeletal reorganization are the hallmarks of epithelial-mesenchymal transition (EMT) [9].
In contrast to E-cadherin, N-cadherin is found in non-epithelial tissues and is expressed in various cell types, including nerve cells, endothelial cells, stromal cells, and osteoblasts. N-cadherin acts as a marker of ongoing EMT. N-cadherin supports angiogenesis and blood vessel integrity by lining endothelial and mural cells, which help to stabilize microvessels. Loss of N-cadherin leads to increased pancreatic intraepithelial neoplasia, indicating that N-cadherin could function as a growth suppressor [15].
In this study, to clarify the pathophysiological function of the role of bile duct epithelial virus infection followed by the process of Epithelial-Mesenchymal Transition (EMT) resulting in BA, we examined and explained the mechanism using mice as our experimental model.
Experimental
Study design
The study design was pure experimental research with "factorial" designs in experimental animals. The experimental unit was some newborn Balb/c mice from a healthy mother. The number of replications was determined based on Federer's formula [16]. Simple randomization was divided into study (KC) and control (KK) groups. The KK has intraperitoneally induced 50 µl phosphate E-buffered saline, while the KC with 50 µl buffered phosphate saline containing 1.5 x 106 fluorescenc E-forming units of Rotavirus Rhesus (American Type Culture Collection, MMU 18006 strain) within the first 24 hours after birth. Some were randomly selected for termination on the 3rd, 7th, 14th, and 21st days after induction.
EMT was measured by calculating the ratio of E-cadherin and N-cadherin (E/N-cadherin) expressions. E-cadherin and N-cadherin expressions of liver and bile ducts of mice after termination were measured quantitatively with BD FACSCalibur flow cytometry and analyzed by BD cell Quest Pro software (Santa Cruz Biotechnology), with a percent unit (%).
Ethical clearance
The study has obtained ethical approval from the Health Research Ethics Committee of the Faculty of Medicine, University of Brawijaya, Malang, Indonesia (No. 361/EC/KEPK-S3/11/2012).
Statistical analysis
The numerical data was normality analyzed first. T-test or Mann Whitney was used for the univariate test, and then inferentially analyzed using multivariate ANOVA (MANOVA) factorial or Kruskal Wallis to analyze the interaction between induction effect of RRV and time range after exposure to E-cadherin and N-cadherin expressions. The statistical analyses were performed utilizing the SPSS software, with a p-value of less than 0.05 interpreted as statistically significant.
Results and discussion
The samples were 48 Mus musculus/Balb c. Obtained two baby mice from KK who died and seven baby mice from KC, so the total samples analyzed were 39 mice babies. The mean initial weight of baby mice was 1.82 grams (heterogeneity p = 0.2).
The median value of E-cadherin in each group of variables between KC and KK was generally different with p <0.05 (Table 1), so as the median N-cadherin values (Table 2). The ratio of E-cadherin and N-cadherin (E/N-cadherin) expressions is also significantly different between the two groups (p <0.05) (Table 3).
Mice babies in KC experience a relatively lower weight gain than in KK. This is following previous studies which found that induced RRV-induced infants had significantly lower weight loss than controls [15]. A separate study reported that almost 80% of neonatal mice infected with RRV experienced jaundice by day 7, ceased weight increase, and succumbed within three weeks. Despite the mortality rate reaching 100%, the precise etiology of death remains uncertain, as the observed mice were no longer infected with the virus [16]. Mortality in KC was more common, especially between days 14 and 21, due to the illness. This is following previous studies that received more than 22% of RRV-induced mice had been dying on the day 21st [17,19-20].
Some of the samples, on histopathologic examination, have demonstrated total clearance, and all of the samples have seen a total visible impairment at termination days to 21. Petersen (1998) and Leonhardt (2010) received a total obstruction after the 14th day [19,20].
Until now, the proof of the hypothesis that EMTs play a role in BA is still being investigated, and relatively few studies have examined changes in cadherin expression (cadherin switch) in BA. EMT in BA is triggered by a chronic inflammatory response mediated by inflammatory cells, and fibroblasts will be activated to trigger MES. Suppose the inflammatory process is acute and the inflammatory process can be stopped. In that case, the EMT process will stop, resulting in the resolution of the MES formed. However, if chronic extensive fibrosis occurs, it results in channel obstruction and malfunction, which, in the end, results in failed organ function [13,22-23].
Decreased E-cadherin expression and N-cadherin increase significantly in KC compared with KK. Harada (2009) stated that administering dsRNA analogs to bile duct cell epithelial cultures decreased E-cadherin expression. The decrease in E-cadherin levels and the concurrent increase in N-cadherin expression in epithelial cells suggest the initiation of the EMT pathway [24].
The E/N-cadherin ratio in KC is lower than that of KK. The ratio or ratio between E-cadherin and N-cadherin expressions to recognize the shifting of cadherin markers, the smaller the ratio or the ratio indicates the occurrence of the marker shift from E-cadherin to N-cadherin. The shift of cadherin expression is a significant sign that the EMT process occurs in the tissues or organs. Araki (2011) received a shift of cadherin expressions from E-cadherin to N-cadherin, invitro-induced by TGF-β induction [17,25].
Conclusion
Induction and long exposure to rotavirus rhesus affect E-cadherin and N-cadherin expressions in mice using the biliary atresia model. The shift of E-cadherin and N-cadherin expressions became the main sign of EMT, which was another study finding. Epithelial to mesenchymal transition, a biological process that causes tissue fibrosis, may contribute to BA pathogenesis.
Acknowledgments
None.
Funding
None.
Authors' Contributions
The author contributed to all research processes, including preparation, data collection, data analysis, and approval for publication of this manuscript.
Conflict of Interest
The authors declare no competing interests related to this study.
Orcid:
Bagus Setyoboedi*: https://orcid.org/0000-0002-3923-6913
Lukman Oktadianto: https://orcid.org/0009-0002-3275-5339
Rendi Aji Prihaningtyas: https://orcid.org/0000-0002-7582-7892
Syania Mega Octariyandra: https://orcid.org/0009-0004-1809-6511
Sjamsul Arief: https://orcid.org/0000-0002-6372-2460
-----------------------------------------------------------------------------------
How to cite this article: Bagus Setyoboedi, Lukman Oktadianto, Rendi Aji Prihaningtyas, Sjamsul Arief. Changes of E-cadherin and N-cadherin expressions in the mice model biliary atresia. Journal of Medicinal and Pharmaceutical Chemistry Research, 2024, 6(8), 1167-1172. Link: https://jmpcr.samipubco.com/article_193249.html
-----------------------------------------------------------------------------------
Copyright © 2024 by SPC (Sami Publishing Company) + is an open access article distributed under the Creative Commons Attribution License(CC BY) license (https://creativecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.

.png)
.png)
