Document Type : Original Research Article
Authors
- Tito Sumarwoto 1, 2
- Heri Suroto 3
- Dwikora Novembri Utomo 3
- Cita Rosita Sigit Prakoeswa 4
- Damayanti Tinduh 5
- Hari Basuki Notobroto 6
- Nur Arfian 7
- Fedik Abdul Rantam 8
- Sholahuddin Rhatomy 9
- Muhana Fawwazy Ilyas 10
- Ferdiansyah Mahyudin 3
1 Doctoral Program of Medical Science, Faculty of Medicine, Universitas Airlangga, Surabaya, East Java, Indonesia
2 Department of Orthopaedic and Traumatology, Prof. Dr. R. Soeharso Orthopaedic Hospital, Faculty of Medicine, Universitas Sebelas Maret, Surakarta, Central Java, Indonesia
3 Department of Orthopaedic and Traumatology, dr. Soetomo General Hospital, Faculty of Medicine, Universitas Airlangga, Surabaya, East Java, Indonesia
4 Department of Dermatology and Venereology, dr. Soetomo General Hospital, Faculty of Medicine, Universitas Airlangga, Surabaya, East Java, Indonesia
5 Department of Physical Medicine and Rehabilitation, dr. Soetomo General Hospital, Faculty of Medicine, Universitas Airlangga, Surabaya, East Java, Indonesia
6 Department of Epidemiology, Biostatistics, Population Studies and Health Promotion, Faculty of Public Health, Universitas Airlangga, Surabaya, East Java, Indonesia
7 Department of Anatomy, Faculty of Medicine, Public Health, and Nursing, Universitas Gadjah Mada, Yogyakarta, Indonesia
8 Virology and Immunology Laboratory, Department of Microbiology, Faculty of Veterinary Medicine, Universitas Airlangga, Surabaya, East Java, Indonesia
9 Department of Orthopaedic and Traumatology, dr. Soeradji Tirtonegoro General Hospital, Faculty of Medicine, Universitas Gadjah Mada, Yogyakarta, Indonesia
10 Department of Neurology, Faculty of Medicine, Universitas Sebelas Maret, Surakarta, Central Java, Indonesia
Abstract
Peripheral nerve injury often results in significant functional impairments, yet effective treatments remain limited. While Adipose-derived mesenchymal stem cells (AdMSCs) hold promise for nerve regeneration, their neurogenic potential remains suboptimal. This study investigates whether platelet-rich plasma (PRP) can enhance the neurogenic differentiation and proliferation of AdMSCs under in vitro conditions. The AdMSCs were isolated and harvested from the abdominal fat tissue of male white rats. These cells were cultured in the third passage and were characterized by specific cell markers. Immunofluorescence staining was utilized to assess CD14, CD45, CD90, and CD105 markers on AdMSCs. The PRP was then prepared from the blood of other rats. Subsequently, the AdMSCs were cultured in neuro-inductive conditioned media plus 10% PRP (experimental group), and Schwann cells were used for control. Then, immunofluorescence staining was conducted for both Schwann-like cells (SLCs) and Schwann cells to visualize b-III tubulin, GFAP, and S100 expression. The result shows that the platelet count in PRP was (1152.81 ± 142.45) x 109/l was significantly higher when compared to the platelet count of venous blood (181.01 ± 22.50) x 109/l (p=0.000). The isolation and characterization of AdMSCs were further successful, confirmed by CD90 and CD105 markers that were positive. Subsequently, the administration of PRP successfully encouraged the AdMSCs proliferation into SLCs. After two weeks of neurogenic induction, PRP-treated AdMSCs showed the same GFAP, S100, and b-III tubulin figures compared to Schwann cells. In conclusion, PRP may be able to promote cell proliferation and neurogenic differentiation of AdMSCs.
Graphical Abstract
Keywords
- Adipose-derived mesenchymal stem cells
- differentiation
- in vitro
- platelet-rich plasma
- Schwann-like cells
Main Subjects
Introduction
Traumatic injuries to the peripheral nerve system are extremely prevalent and may result in serious functional issues. Between 2009 and 2018, the incidence rate of these injuries climbed to 36.9 per 1,000,000 person-years [1]. Despite the inherent regenerative capacity of the peripheral nervous system, it is uncommon for injured nerves to return to a completely normal state, even following surgical treatment. Normal function typically does not return after surgery, or it takes an enormous length of time due to several factors, including the inflammatory response and the formation of fibrous tissue [2]. In recent years, as a result of advancements in stem cell research, regenerative treatment has been employed to manage various peripheral nervous system injuries. The objective is to generate functional tissue to repair or replace damaged organs or tissue function. Multiple studies have revealed the potential application of stem cell-based biomedical techniques in the treatment of damage to the peripheral nervous system [3,4].
Schwann cells have been utilized to treat peripheral nerve injuries. However, the use of autologous Schwann cells has several drawbacks, including the need for surgery to collect, the difficulty of culturing and reproducing in sufficient quantities, the length of time required to obtain sufficient cells, the high purity level required for Schwann cells transplantation, as well as morbidity at the donor site. Meanwhile, the use of allogeneic or xenogenic Schwann cells can also result in immunological rejection [3]. In peripheral nerve regeneration, undifferentiated stem cells have been utilized extensively; compared to Schwann cells, these cells have a high ability for proliferation. Undifferentiated stem cells can differentiate into many types of specialized cells, including Schwann cells. The most commonly employed forms of stem cells include bone marrow-mesenchymal stem cells (BM-MSCs) and adipose-derived mesenchymal stem cells (AdMSCs), as well as umbilical cord tissue-mesenchymal stem cells (UC-MSCs), which can be obtained by autograft or allograft. Previous studies showed that stem cells have significant clinical potential and can be utilized in cell-based tissue engineering [3,5].
From the various sources of stem cells, adipose tissue is known to be the most suitable for clinical applications. The tissue can obtained from a by-product of plastic surgery, especially as the popularity of liposuction grows. The pluripotency and proliferative potential of adipose-derived stem cells were comparable to those obtained from bone marrow. It has also been demonstrated that they possess neuronal differentiation capabilities to become Schwann-like cells (SLCs). Several animals have demonstrated their potential in nerve regeneration applications [5,6]. Most studies show that these cells exert augmentation effects after being implanted in silicon conduits. In particular, transplantation of these cells may also reduce muscle atrophy frequency, promote axon formation and myelination processes, and reduce inflammation [7]. Besides, the extraction of stem cells from other sources, for instance, bone marrow, necessitates invasive and potentially painful biopsies, the number of stem cells produced is relatively low, and their maximal lifespan diminishes with age [5,6].
However, the AdMSCs ability to proliferate and differentiate into neurogenic cell lines (SLCs) is not as powerful as stem cells obtained from the peripheral nervous system. To address this limitation and enhance the therapeutic potential of AdMSCs, platelet-rich plasma (PRP) has emerged as a promising adjunct in in vitro cell culture systems. The therapeutic effect of PRP is known to depend on various growth factors released from activated platelets, such as transforming growth factor (TGF)-β, platelet-derived growth factor (PDGF), vascular endothelial growth factor (VEGF), and stromal cell-derived factor (SDF)-1α. Previous study shows that the PRP and its numerous growth factors have been demonstrated to stimulate neurogenic differentiation and cell proliferation in vitro, although research is limited [6].
Therefore, this study was designed to investigate whether PRP can effectively promote neurogenic differentiation and proliferation of AdMSCs under in vitro conditions. By addressing this question, we aim to elucidate the potential of PRP as a supplement to enhance the regenerative capacity of AdMSCs for peripheral nerve regeneration.
Experimental
Study design
This is an experimental study with in vitro design performed at the Animal and Stem Cell Research Institute of Tropical Disease Laboratory, Universitas Airlangga, Surabaya, Indonesia, as well as the Anatomy-Histology Laboratory, and the Anatomic Pathology Laboratory, Faculty of Medicine, Public Health and Nursing, Universitas Gadjah Mada, Yogyakarta, Indonesia. According to ethical standards and practices, all procedures and data collection have been approved by a local institutional review board, Animal Care and Use Committee (ACUC), Faculty of Veterinary Medicine, University Airlangga, Surabaya, East Java, Indonesia) with the letter number of 2.KE.038.05.2020 on May 13, 2020.
Isolation and characterization of AdMSCs
Two white male rats, Rattus norvegicus with Wistar strain, aged 3 to 4 months and weighing 200 to 300 grams, were used for the AdMSCs isolation. Animals were housed in standard conditions. The rats were sacrificed, then the abdominal fat pad was taken, and AdMSCs were isolated according to Zuk et al. (2001) and Gimble et al. (2007) techniques [8,9]. The adipose tissue obtained from the abdomen was washed with Phosphate-Buffered Saline (PBS) to remove the blood and then was cut into 1 mm × 1 mm sizes and was digested by collagenase I. Subsequently, adipose tissue was separated mechanically for 80 min at 37 C using 0.1% collagenase I (Gibco). Then, the suspension was centrifuged to separate the floating adipocytes from the stromal vascular fraction (SVF). The cells in the normal vascular fraction were then maintained at 37 C with 5% CO2 in Dulbecco's modified Eagle's medium (DMEM, Gibco) supplemented with 10% FBS (Gibco)/1% penicillin-streptomycin/2 mM L-glutamine, incubated in a moist atmosphere and 5% CO2 at 37 °C for 48 hours. The medium containing non-adherent cells was then removed and replaced with a fresh culture medium, and then AdMSCs cells were passaged and used after passage three until six times. Finally, to confirm the cellular identity of cultured AdMSCs cells, CD14, CD45, CD90, and CD105 immunofluorescence staining was examined on AdMSCs from passage 3 [6,10].
Collection and preparation of PRP
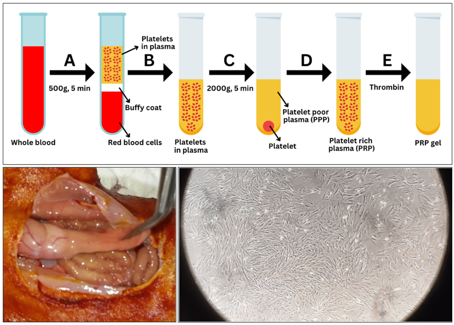
The PRP was collected and prepared from three experimental animals (Figure 1). Rats were anesthetized, and blood was taken and collected by inserting a needle intracardiac. The experimental animals were then sacrificed by injecting intracardiac sodium pentobarbital. All blood obtained was added to the anticoagulant, citrate phosphonate dextrose (CPD) buffer in 0.15 mg/ml blood with a 1 ml CPD buffer ratio to 5 ml blood. After that, it was centrifuged at 500 g for 5 minutes at 25 C. The supernatant containing PRP was then used for a second centrifugation at 2000 g for 5 min at 25 C. The pellet from the second centrifugation was saved and diluted with the supernatant until the platelet concentration was 1.5 x 1012 platelets/L [11].
Schwann-like cells (SLCs) differentiation of AdMSCs
The preparation of SLCs derived from AdMSCs was performed using an administration of 10% PRP. In the third passage, the AdMSCs cells were differentiated into a SLCs (differentiated AdMSCs/dAdMSCs) phenotype in two initial steps and then followed by administration of 35 ng/ml all-trans-retinoic acid (Sigma-Aldrich) for 72 hours. After that, cells were treated with differentiation media consisting of growth medium supplemented with 5 ng/ml PDGF (PeproTech), 10 ng/ml basic fibroblast growth factor (bFGF) (PeproTech), 14 μM forskolin (Sigma-Aldrich), and 252 ng/ml neuregulin-1 (R&D System) as well as PRP for a minimum of 14 days prior to characterization. The added growth factors were selected based on their role in modulating Schwann cells development and survival [12]. The SLCs-differentiated AdMSCs utilized in this study were cells in passages 3-6. The O2 concentration in the chamber was controlled by the ProOx-C-chamber 110 model at 21%, which was well characterized and controlled (Biospherix, Redfield, New York) for 24 hours [13]. AdMSCs in passage three were harvested and seeded in 96-well culture plates with the same cell count of 5,000/ml for proliferation assay. The cell count kit (CCK)-8 test was carried out sequentially for six days to obtain a growth curve. The culture medium used in the 96-well plate was the same as that used in the neural inductive culture system.
Collection and preparation of Schwann cells
Schwann cells were harvested from the sciatic nerve of the three-month-old white male rats. The sciatic nerve was cut ~1 cm, and the epineurium was detached. The sciatic nerve was chopped into small pieces about 1 mm long and separated by enzyme collagenase NB4 (2 g/ml; 17,454; SERVA) dispersed in DMEM/F-12 for 15 min at 37 °C, centrifuged, and resuspended in DMEM/F-12 consisting 10% fetal bovine serum. The cells gained by this procedure were cultured in an incubator at 37 °C under a 5% CO2 atmosphere. Following 48 h, the supernatant was separated, and the cells were resuspended in 1 mg/mL collagenase NB4 to refine these cells from fibroblasts. Refined SC was utilized for all following experiments [14].
Data outcome measures
Platelet quantification in PRP was achieved by counting the hemocytometer. At the same time, immunofluorescence staining was utilized to assess CD14, CD45, CD90, and CD105 markers on AdMSCs. Immunofluorescence staining was also conducted for SLCs and Schwann cells to visualize b-III tubulin, GFAP, and S100 expression. The procedures involved fixation, permeabilization, blocking, and subsequent incubation with primary and secondary antibodies, with visualization carried out using fluorescence microscopy collectively.
Statistical analysis
Data were presented as mean and standard deviation. Shapiro-Wilk test was used to define the distribution of data. An independent t-test was used to assess the differences between platelet count in venous blood vs. in PRP. Data were analyzed using Statistical Package for the Social Sciences (version 27.00) for statistical analysis software (IBM Corp, Armonk, New York, USA). P<0.05 (with a confidence limit of 95%) was considered statistically significant.
Results and discussion
Comparison of platelet concentrations in venous blood and platelet-rich plasma
The platelet count in PRP (1152.81 ± 142.45) x 109/l was significantly higher when compared to the platelet count of venous blood, which was (181.01 ± 22.50) x 109/l (p=0.000). The average platelet density in PRP increased by 636.88% compared to venous blood.
Characterization of AdMSCs
Isolation of AdMSCs was derived from two white rats of Rattus norvegicus Wistar strain, male, aged 3-4 months and weighing around 300 grams. Adipose tissue was taken to isolate adipose mesenchymal cells. The rats were anesthetized according to the procedure; the abdominal fat pad was then taken (Figure 2A). The AdMSC cells were passaged and used after passage 3-6 times (Figure 2B). Immunofluorescence staining was performed for CD14, CD45, CD90, and CD105 in AdMSCs from passage 3 to ascertain the cellular specification of the cultured AdMSC cells (Figure 3). After 15 days of incubation in DMEM medium and after reaching 80% confluency in an incubator of 37 °C 5% CO2 95% air, the AdMSCs were harvested and examined using immunohistochemistry with the result of positive for CD 90 and CD 105, but negative for CD 14 and CD 45.
The effect of PRP on SLCs differentiation
Preparation of SLCs derived from AdMSCs of rats using the protocol from Kingham by administering 10% PRP. In the third passage, AdMSCs cells were phenotypically differentiated into SLCs (Schwann-like cell-differentiated AdMSCs/dAdMSCs), and then the expression of GFAP, b-III Tubulin, and S100 proteins was examined. After two weeks of neurogenic induction into SLCs and two weeks of isolation and culture of rat sciatic nerve-derived stem cells, the expression of GFAP, b-III Tubulin, and S100 proteins was examined by immunofluorescence examination in both of these cells (Figure 4).
Discussion
This study shows that the platelet count in PRP was significantly higher than that of venous blood. Subsequently, the isolation and characterization of AdMSCs were successful, confirmed by CD14 and CD45 markers, which were negative, while CD90 and CD105 were positive. CD14 and CD45 are markers for monocytes and mononuclear cells, respectively [15,16], and negative expression in these AdMSCs suggests that they are not of hematopoietic lineage. On the other hand, CD90 and CD105 are markers for MSCs [17], and their positive expression in these AdMSCs indicates that they are likely to be MSCs.
The AdMSCs have a great ability to undergo multidirectional differentiation, including differentiation into SLCs [18-20]. Previous studies have shown that the PRP addition has been shown to stimulate the proliferation of AdMSCs cells in vitro and has significant potential to promote SLCs differentiation. This PRP effect can facilitate the potential use of AdMSCs for peripheral nerve regeneration processes. The mechanism of PRP therapy is related to various growth factors released from activated platelets. These cytokines can stimulate cell growth, migration, mobilization, and differentiation. Through these growth factors, PRP can exert its ability to encourage the regeneration of peripheral nerve tissue [6]. Several protein expressions are known to be used to prove the existence of an SLCs phenotype, which is the result of the neurogenic induction of AdMSCs, including MAP-2, b-III tubulin, S-100, GFAP, Nestin, NSE, TAU, Synaptophisin, GAP-43, NCAM, and SYN1 [6,21]. In this study, an examination of the expression of GFAP, tubulin III, and S100 proteins was carried out to prove the presence of neurogenic induction of AdMSCs to become SLCs after two weeks of induction. This is indicated by the appearance of cells' immunofluorescence (greenish glow). As a result, the administration of PRP into culture media encouraged the proliferation of AdMSCs into SLCs in this study, as proved by after two weeks of neurogenic induction, PRP-treated AdMSCs showed the same GFAP, S100, and b-III tubulin figures compared to the Schwann cells.
GFAP is a marker for astrocytes, a glial cell in the central nervous system. It is involved in maintaining the blood-brain barrier, providing structural support, and regulating the extracellular environment. GFAP is a marker of maturation and myelination in the context of Schwann cells [22]. Subsequently, S100 is a calcium-binding protein that is present in the central nervous system, including glial and Schwann cells. It stimulates cellular processes such as proliferation, differentiation, and survival. In Schwann cells, S100 is involved in myelination and the regulation of axonal growth [23]. In addition, b-III tubulin is a microtubule-associated protein that plays a crucial role in the formation and maintenance of microtubules, which are essential for cellular structure and function. In Schwann cells, b-III tubulin is involved in the organization of microtubules during myelination [24].
AdMSCs have great potential for tissue repair and regeneration [25,26]. AdMSCs are usually isolated by enzymatic digestion, filtration, and centrifugation. They are usually expanded in monolayers on standard tissue culture plastic with basal media containing 10% FBS, which is important in cell culture [27]. However, FBS remains unsafe when cultured cells are used in regenerative medicine. Serums of animal origin may contain xenoproteins, which may cause rejection and contain infectious agents that may transmit. To eliminate the use of animal products in human AdMSCs cultures, PRP can be used instead of FBS because PRP contains various growth factors, proteins, and enzymes that support cell growth and proliferation [28-30]. In previous studies, PRP alone has been shown to contain a 3- to 5-fold increase in growth factor concentrations [31,32]. PRP has the potential to improve healing with the presence of various growth factors and cytokines from α granules contained in platelets. Growth factors identified in platelets include TGF-β, PDGF, IGF-I, IGF-II, fibroblast growth factor (FGF), epidermal growth factor (EGF), and VEGF. These growth factors play an important role in cell proliferation, chemotaxis, cell differentiation, and angiogenesis [32].
In clinical use, platelet concentrates are also known to have many advantages. When used as a supplementary medium, PRP was shown to increase the growth of AdMSCs and maintain their differentiation. Furthermore, PRP's antimicrobial and anti-inflammatory properties are valuable adjuncts for enhancing tissue regeneration. Wound healing processes and neovascularization in a pig model are increased when AdMSCs are administered topically together with PRP, and these effects are largely due to the large number of growth factors found in PRP [30,33]. In addition, the regenerative potential of platelet concentrates and AdMSCs in hard and soft tissues has been investigated in recent years. Preclinical studies in animal models have shown AdMSCs and PRP synergistic effects in wound healing [34] and osteoarthritis [35,36]. A study conducted by Cervelli et al. reported that the combination of PRP, autologous AdMSCs, and hyaluronic acid as a wrap to regenerate tissue and achieve localized wound epithelialization in the lower limbs obtained a significant reduction in healing time in most of the 30 patients treated. Subsequently, Cervelli et al. also reported less use of a number of drugs and an increase in quality of life [37].
Pak and colleagues also injected AdMSCs and PRP in 91 patients with various orthopedic pathological conditions. The follow-up for up to 30 months showed that the procedure was safe, as tumors did not appear at the injection site [38]. A study by Bui et al. was also performed on 21 patients with grade II to III osteoarthritis. This group aimed to demonstrate the clinical safety and efficacy of autologous transplantation of AdMSCs in combination with PRP. The result was a total reduction in pain level in 100% of patients without complications, such as tumor formation or microorganism infection [39]. Overall, these studies highlight the great potential of AdMSCs in combination with PRP as therapeutic agents in regenerative medicine.
Limitations of study
This study solely focuses on in vitro conditions, which may not fully mimic the complexities of the in vivo environment. Furthermore, the study primarily focuses on a limited set of markers (CD14, CD45, CD90, CD105, b-III tubulin, GFAP, and S100) to assess cellular differentiation and expression. This limited marker panel might not fully capture the complexity of cellular changes and interactions occurring during neurogenic differentiation. Subsequently, examination of each marker was only performed qualitatively using immunofluorescence. The study included a quantitative examination in the future may be beneficial. Finally, variation in responses might arise when using cells from different individuals due to inherent biological diversity.
Conclusion
This in vitro study indicates that PRP administration has the potential to promote the proliferation of AdMSCs and neurogenic differentiation into SLCs, as evidenced by PRP-treated AdMSCs showed the same figures of GFAP, S100, b-III tubulin compared to the Schwann cells. Based on these findings, PRP appears to have the potential to promote the proliferation and neurogenic differentiation of AdMSCs, making them a more viable option for peripheral nerve regeneration.
The practical significance of these results lies in the potential clinical applications for peripheral nerve repair and regeneration. If validated using in vivo studies and clinical trials, combining PRP and AdMSCs could emerge as a valuable strategy in regenerative medicine. This approach may offer clinicians a reliable method for enhancing peripheral nerve repair outcomes, potentially leading to improved functional recovery and quality of life for patients with peripheral nerve injuries. However, it's crucial to acknowledge the need for further research to validate these findings in more clinically relevant settings and to address any potential study limitations.
Acknowledgments
We would like to express our sincere gratitude to Brigitte Rina Aninda Sidharta, dr. SpPK(K), for her invaluable expertise and dedicated efforts in conducting the laboratory analysis and providing insightful interpretations for this manuscript. Her contributions have greatly enriched the scientific rigor and depth of this study.
Funding
None.
Authors' Contributions
T.S., F.M., H.B.N.: Conceptualization, study design, performed experiments, data analysis and interpretation, data curation, formal analysis, funding support, investigation, methodology, project administration, resources, validation, visualization, writing original manuscript draft, critical review, editing and approval of the final version of the manuscript. T.S., H.S., N.A., C.R.S.P., D.T., M.F.I.: performed surgery and experiments, data collection, analysis & interpretation, critical review. editing and approval of final version of the manuscript. data curation, formal analysis, investigation, visualization, writing, review and editing. H.S., F.A.R.: microsurgery advice, critical review, editing and approval of final version of the manuscript. D.N.U., H.S., F.M.: Scientific and microsurgery advice from clinical perspective, and critical review, editing and approval of final version of the manuscript. S.R., F.M.: resources, scientific/protocol advice, critical review, editing of final version of the manuscript. All authors approved of the full manuscript.
Conflict of Interest
None.
Orcid:
Tito Sumarwoto*: https://orcid.org/0000-0002-1403-6667
Heri Suroto: https://orcid.org/0000-0002-9384-897X
Dwikora Novembri Utomo: https://orcid.org/0000-0002-7832-5695
Cita Rosita Sigit Prakoeswa: https://orcid.org/0000-0003-3232-095X
Damayanti Tinduh: https://orcid.org/0000-0001-6604-8152
Hari Basuki Notobroto: https://orcid.org/0000-0002-3905-7413
Nur Arfian: https://orcid.org/0000-0003-1694-2054
Fedik Abdul Rantam: https://orcid.org/0000-0001-8182-1465
Sholahuddin Rhatomy: https://orcid.org/0000-0002-5512-6706
Muhana Fawwazy Ilyas: https://orcid.org/0000-0002-0176-9773
Ferdiansyah Mahyudin: https://orcid.org/0000-0001-8757-9251
--------------------------------------------------------------------------------
How to cite this article: Tito Sumarwoto, Heri Suroto, Dwikora Novembri Utomo, Cita Rosita Sigit Prakoeswa, Damayanti Tinduh, Hari Basuki Notobroto, Nur Arfian, Fedik Abdul Rantam, Sholahuddin Rhatomy, Muhana Fawwazy Ilyas, Ferdiansyah Mahyudin, Enhancement of Schwann-like cells differentiation from adipose-derived mesenchymal stem cells by administration of platelet-rich plasma: An in vitro study. Journal of Medicinal and Pharmaceutical Chemistry Research, 2024, 6(9), 1383-1394. Link: https://jmpcr.samipubco.com/article_194465.html
--------------------------------------------------------------------------------
Copyright © 2024 by SPC (Sami Publishing Company) + is an open access article distributed under the Creative Commons Attribution License(CC BY) license (https://creativecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.

.png)
.png)
.png)
.png)
