Document Type : Case Report
Authors
Department of Anesthesiology and Reanimation, Faculty of Medicine, Universitas Airlangga, Dr. Soetomo Genaral Academic Hospital, Surabaya, Indonesia
Abstract
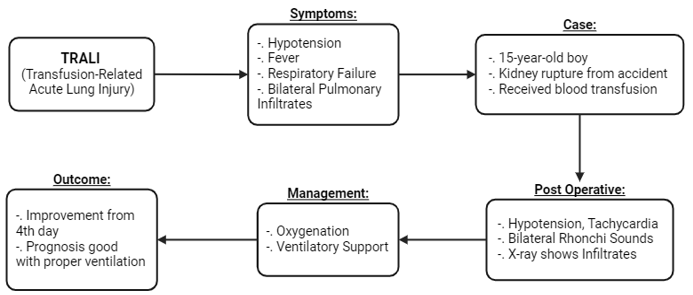
Within 6 hours post-blood product transfusion, TRALI manifests as non-cardiogenic pulmonary edema. Bilateral pulmonary infiltrates, hypotension, fever, and respiratory failure are potential clinical manifestations. A 15-years-old boy underwent surgical resuscitation after a traffic accident which caused grade 5 kidney rupture, nephrectomy was then performed. Intraoperatively the patient received a transfusion of 800 mL whole blood and 600 mL packed red cell. Post-operatively, there was hypotension, tachycardia, and PCV mode ventilator was installed with bilateral rhonchi breath sounds. Supporting the diagnosis of TRALI, the chest x-ray revealed bilateral infiltrates. In this case, the risk factors for TRALI are the quantity of units transfused and the utilization of mechanical ventilation. Supportive management in the form of adequate oxygenation and ventilatory support resulted in a good outcome where the patient was improving from the 4th day post-operative. In accordance with the literature, the TRALI prognosis with adequate ventilator management is good.
Graphical Abstract
Keywords
Main Subjects
Introduction
While blood transfusion proves life-saving for those facing blood loss or impaired production, it is not without risks. The decision to transfuse a patient necessitates careful consideration of potential complications associated with this intervention [1]. Transfusion-related acute lung injury (TRALI), categorized as a new-onset acute lung injury (ALI), emerges approximately six hours post-blood product transfusion and is distinct from cases influenced by other risk factors. On the other hand, delayed TRALI occur in longer window time period, defined as 72 hours from transfusion is completed [2]. The primary source of morbidity and mortality associated with blood transfusion among numerous potential complications is TRALI [3]. Reportedly, in the United States, TRALI occurs in 1 out of every 5000 patients who undergo blood product or blood component transfusion. It stands as the fourth most prevalent adverse transfusion reaction and the third leading cause of death [4]. The risk of TRALI is higher in those with ARDS, cardiac comorbidity, or existing lung injury [2].
The complete elucidation of TRALI's pathogenesis remains elusive to date [5]. Sudden non-cardiac pulmonary edema, manifesting as acute respiratory distress, stands as a common symptom frequently reported by some patients with TRALI. The swift identification and treatment of hypoxemia, a significant complication of TRALI, are imperative [4]. The primary management of TRALI is supportive care. Suspected blood products should be stopped immediately. Oxygen supplementation is imperative for all TRALI patients. Moreover, mechanical ventilation becomes necessary in 70-90% of cases. To effectively manage patients with ALI, the application of restrictive tidal volume ventilation is considered crucial to prevent lung injury exacerbation. Nevertheless, alternate treatment approaches for this disease have not been conclusively identified to date. Although therapeutic options derived from G2A receptor studies have been disclosed, their results remain inconclusive. Definitive measures to avert new TRALI incidents are currently unavailable as the pathophysiology and etiology are not yet fully understood, in addition to the unavailability of rapid diagnostic tests [5].
Case report
A 15-years-old boy presented after traffic accident. He was wearing a helmet and there was no history of fainting, bleeding from neither nose, nor ears since the incident. The patient experienced pain on the left flank. The patient was then taken to Anwar Medika Regional Hospital with vital signs showing normotension, tachycardia, and GCS E3M5V6. Fluid resuscitation, whole blood transfusion, tranexamic acid injection, ceftriaxon injection, ketorolac injection, and tetagam were given, and then the patient was referred to RSDS. On primary survey, he was alert, with free airway, spontaneous breathing, RR 26 x/minute, blood pressure 110/60 mmHg, pulse 135 regular x/minute, CRT 2 seconds, SpO2 98-99% with O2 nasal cannula 3 lpm. Physical examination revealed distended abdomen and an open wound in the left flank area measuring 6x5 cm, irregular edges, with abrasion around the wound, which seemed to penetrate the fascia and suspected involvement of the left kidney (Figure 1), there was tenderness throughout the abdomen. Examination of the head, neck, thorax, urogenital and extremities were within normal limits.
Initial laboratory tests showed hemoglobin 3.7 g/dl, hematocrit 11.0%, platelet 106,000/dl, CRP 2.53, serum creatinine 1.62, and albumin 2.79. FAST ultrasound revealed the presence of free Morison's pouch fluid, right paracolica, suggesting renal rupture. Head CT scan, pelvic X-ray, and chest X-ray without contrast were normal.
The patient is then prepared for surgical resuscitation. The patient was diagnosed as ASA 4D, with massive bleeding, severe anemia, abdominal distension, and increased renal function. General anesthesia was performed with induction using ketamine 50 mg and rocuronium 50 mg. The patient was intubated with a cuffed ETT 7.0 with etCO2 (+) 32 mmHg. Maintenance anesthesia was carried out by administering ketamine syringe pump 50 mg/hour and Sevoflurane 2 vol% + O2 + water.
Intraoperative hemodynamics showed BP 75-130/38-88 mmHg, HR 95-140 x/minute with NE 50-100 ng. During the operation the patient received RL 1,000 mL, NS 500 mL, whole blood transfusion 800 mL and PRC 600 mL. Intraoperative findings showed peritoneal fluid mixed with blood ± 1,000 mL, intact spleen and liver, active bleeding from the left renal pedicel, shattered left kidney (grade V renal rupture). Left nephrectomy was then performed. Postoperative hemodynamics was stable but the patient then cardiac arrest occurred, so cardiopulmonary resuscitation was performed for 3 minutes resulting in ROSC. Rapid AF occurred post ROSC with a heart rate of 160-200 x/minute and BP 80/40 mmHg, then cardioversion of 50 and 100 joules was given and the rhythm returned into sinus tachycardia. Central venous catheter insertion was carried out.
On the first day in the intensive observation room (ROI), PCV mode ventilator was installed and there was bilateral crackles vesicular breath sounds, wheezing (-/-), cold dry pale extremities, BP 85-102/45-65 mmHg with NE 100-150 ng, and pulse 130-140 x/minute. Blood gas analysis was carried out (Table 1). A chest X-ray was performed (Figure 2) and according to the clinical and further work-ups, the patient was suspected to have TRALI.
The medications given are RL 1,500 mL/24 hours, Metamizole 1 g/8 hours, Metronidazole 500 mg/8 hours, Ceftriaxone 1 g/12 hours, Omeprazole 40 mg/12 hours, Metoclopramide 10 mg/8 hours, Tranexamic acid 500 mg/8 hours, Vitamin K 1 ampule/8 hours, Dexamethasone 5mg Inj /8 hours, Rocuronium 20 mg/hour, Midazolam + Morphine 1:1 2 mL/hour, NE according to hemodynamics, and Dobutamine 3 gamma.
On the 2nd day of admission, edema was observed thus furosemide 20 mg was added. On the 3rd day of admission, the ventilator mode was set to PSIMV, bilateral crackle vesicular breath sound was decreased, BP 95-106/59-69 mmHg with NE 50 ng, pulse 105 x/minute. On the 4th day of admission, vesicular breath sounds rhonchi (+/-) was found, BP 98-112/62-76 mmHg without support, and pulse of 90 x/minute. On the 5th day of admission, there were no vesicular crackle breath sounds with the chest x-ray improvement (Figure 3), finally the patient was extubated. After spending seven days in the hospital, the patient transferred to the low-care ward and was discharged two days thereafter.
Discussion
Coined by Drs. Popovsky and Moore in 1985, TRALI is used to denote an acute lung injury (ALI) syndrome linked with transfusion. As per the National Heart Lung and Blood Institute, the diagnosis of TRALI is established when new-onset ALI occurs after transfusion. The manifestation of signs or symptoms takes place while undergoing transfusion or within a 6-hour timeframe thereafter. The American-European Consensus Conference outlines the following criteria for ALI: (1) bilateral infiltrates evident on frontal chest radiograph; (2) pulmonary artery wedge pressure measuring ≤ 18 mmHg upon measurement or the absence of clinical signs of left atrial hypertension; (3) ratio of PaO2/FIO2 ≤ 300 mmHg irrespective of PEEP level (for patients without arterial blood gas data, a hypoxemia criterion is met with oxygen saturation < 90% while breathing room air); (4) and acute onset [6]. The predominant cause of TRALI typically stems from antibodies targeting human neutrophil antigen (HNA) or human leukocyte antigen (HLA) present in transfused blood products. This occurrence is particularly prevalent in patients whose leukocytes express comparable antigens [4,5].
In 2019, the TRALI definition was updated with major modifications, namely: (i) removing the term "possible TRALI"; (ii) Categorizing TRALI into type I (lacking ARDS risk factors) and type II (presenting with ARDS risk factors or pre-existing mild ARDS); (iii) Classifying cases with ARDS risk factors meeting the diagnostic criteria for ARDS, along with respiratory deterioration in the 12-hour period preceding the transfusion, as ARDS instead of TRALI type II; and (iv) Incorporating important updates such as guidance to diagnose hydrostatic pulmonary edema into the revised TRALI definition [7].
According to several studies, TRALI can be caused by damage to lung vascularization associated with neutrophils in the form of HNA or HLA antibodies in donor blood. These antibodies have the propensity to bind to recipient antigens, contributing to the onset of TRALI. Storage of blood products can accumulate Blood product storage has the potential to accumulate pro-inflammatory mediators, constituting an additional factor leading to TRALI. The clinical syndrome adheres to the two-hit hypothesis. In this scenario, neutrophil sequestration takes place in the pulmonary vasculature, where activated neutrophils actively damage the endothelial lining, resulting in the leakage of proteins and fluids into the alveolar spaces [5,8-9].
Risk factors contributing to TRALI can be broadly classified into those related to the recipient and those associated with the transfusion itself. Among recipient-related risk factors, several comorbidities have been identified as potential contributors to TRALI, including excessive alcohol consumption, mechanical ventilation, end-stage liver disease, sepsis, hematological malignancies, coronary artery bypass grafting, and extensive transfusions. One of the most significant risks for TRALI is critical illness. A comprehensive review involving a population of 11 million elderly individuals in the US demonstrated a heightened TRALI incidence in individuals who underwent transfusions, including those receiving platelet or plasma transfusions. An escalation in the TRALI incidence correlates with the quantity of units transfused. In addition, a review highlighted that women between 65 and 79 years old with a history of tobacco consumption and a six-month record of post-inflammatory pulmonary fibrosis faced an elevated risk of developing TRALI [5,8]. In our case, the potential risk factors related to the recipient are mechanical ventilation and critical illness secondary to traffic accident. The TRALI incidence increases with the number of units transfused, as in this case the patient received quite a large transfusion with a total of 800 mL whole blood and 600 mL PRC.
In terms of transfusion-related risk factors, TRALI has been linked to immunoglobulin and stem cell preparations. The association between TRALI and immunoglobulins, as well as stem cell preparations, persists as a noteworthy aspect. In a case-control investigation involving 89 TRALI subjects with 164 controls, a higher odds ratio was reported, indicating an association between TRALI and plasma from female donors, as well as a higher number of transfusions. A heightened TRALI incidence was observed in association with blood products, particularly those with elevated plasma volumes such as platelet concentrate, whole blood, and fresh frozen plasma (FFP). TRALI has been correlated with heightened levels of HNA antibodies. In contrast, there is no association between TRALI and anti-HLA class I or HLA class II antibodies [5,8]. The risk of TRALI is reportedly influenced by the age of blood products. While numerous studies have highlighted that the storage of red blood cells can induce morphological and biochemical alterations termed red blood cell storage lesions, it is noteworthy that two studies conducted to date have not affirmed blood product age as a confirmed risk factor for TRALI [5,8]. Our patient received whole blood and PRC transfusion intraoperatively. According to the literature, there is an elevated incidence of TRALI associated with whole blood transfusion. While TRALI is commonly linked to plasma from female donors and a higher number of transfusions, in this case the identity of the donor is unknown, but as previously explained the patient received a high volume of transfusions due to a massive bleeding.
The TRALI incidence is considered rare, and its accurate estimation has been challenging due to several factors. These include the disparities in global reporting mechanisms, irregular use of standardized definitions, and challenges in identifying the syndrome. In historical terms, TRALI was approximated to occur at a frequency of around 1 in 5,000 transfused blood components. The incidence in North America is 1 in 1,333-5,000 per unit transfused, whereas in Europe it varies from 1 in 29,000-270,000 per unit transfused [10]. Quebec's recent report revealed an incidence of 1 in 100,000, while in Europe, the estimated range is from around 1.3 to 1 in 100,000 to 1 in 7,900.4 In the United States, incidents categorized as TRALI and potential TRALI represent the second most prominent reason for transfusion-related mortality, accounting for 24%, following transfusion-associated circulatory overload (TACO) at 34% [11].
The complete understanding of TRALI's pathophysiology remains elusive.
Anti-leukocyte antibodies garnered attention in the 1950s as initial reports linked them to TRALI's pathogenesis. Bilateral pulmonary infiltrates, hypotension, fever, and respiratory failure constitute the clinical manifestations of TRALI. The mechanisms proposed for TRALI involve both non-immune-mediated and immune-mediated pathways [3].
Anti-HLA class I and II antibodies, and less commonly, antibodies targeting granulocyte-specific antigens (HNAs), contribute to immune-mediated TRALI. These antibodies have the potential to be present in either the recipient or donor serum, where they interact with leukocytes from either the donor or recipient. Approximately 65-85% of all TRALI cases are attributed to immune-mediated mechanisms, with HLA-A2 being the most frequently documented among other HLAs. In addition, Associations with TRALI have been observed in cases where antibodies target HLA class II. The immune model faces criticism due to instances where patients undergo transfusion procedures without experiencing TRALI, even though leukocyte antigen is present. This can be explained by heterozygosity of antigen receptors recognized by antibodies. The degree of manifestation of pulmonary transfusion reactions can also be influenced by the recipient's clinical manifestations. Furthermore, the lack of detection by medical personnel plays a role in such cases [3].
Even with the application of sensitive assays, HNA and HLA antibodies are not detected in approximately 20% of TRALI cases involving the transfused product. In these instances classified as "non-antibody-mediated" TRALI, the absence of identified antibodies may arise from interaction with other biological reactive molecules (BRMs) present in the transfused blood component, such as platelet microparticles, pro-inflammatory cytokines, or bioactive lipids. These molecules exhibit high procoagulant activity and tend to accumulate in stored blood components, contributing to the observed cases of TRALI without identified antibodies [3,12].
Polymorphonuclear neutrophils emerge as the primary inflammatory cells engaged in the TRALI pathogenesis. TRALI mechanism heavily relies on the production of leukocyte antibodies. Described as a two-hit theory, the disease pathogenesis involves the interplay of recipient predisposition and the occurrence of adverse elements in blood products [1,13]. In the initial hit, which centers on recipient predisposition, there are polymorphonuclear neutrophils (PMNs) priming and pulmonary endothelial cells (ECs) activation. This sequence ultimately leads to the pulmonary alveolar-capillary permeability barrier being disrupted. In the second hit, stored transfused units contain mediators that trigger primed PMNs, as well as other cells such as ECs, monocytes, macrophages, and platelets. The activation of these cells induces coagulopathy and results in the release of pathogenetic factors, eventually causing fluid intrapulmonary infiltration. Distinguishing between antibody-dependent and -independent TRALI is possible during the second hit by identifying specific pathogenic mediators in the blood components. The pathogenic factors of TRALI are effectively elucidated by the two-hit hypothesis. However, delving deeper into disease pathogenesis reveals three interconnected phases: the priming step, pulmonary reaction, and effector phase [14,15]. In response, activated neutrophils discharge inflammatory mediators, including IL-8, IL-6, IL-1, and TNF-alpha cytokines. Simultaneously, proteolytic enzymes were released, and reactive oxygen species were generated. Initiating a cascade of immune reactions, this event causes harm to the vascular endothelium. Consequently, it leads to the leakage of pulmonary capillary fluid into the alveolar space, resulting in edema [1,7].
Neutrophils primarily contribute to the general pathophysiological pathway of TRALI by causing damage to the alveolar-capillary membrane. Neutrophils trapped in the microvasculature undergo agglutination due to antibodies present in the transfused blood. The capability to induce active neutrophil agglutination is a characteristic of most leukocyte IgG antibodies. Leukocyte antibodies or active lipids stimulate neutrophils, prompting the release of oxygen radicals. These radicals inflict damage on pulmonary capillary endothelial cells, elevate vascular permeability, and eventually lead to the secretion of protein and fluid into the alveoli [3].
Patients with TRALI frequently exhibit acute respiratory failure, characterized primarily by dyspnea. This clinical manifestation is often accompanied by cyanosis, tachycardia, and tachypnea. Additional alterations, including fever, hypotension, or hypertension, have also been documented. In the absence of other risk factors for ALI, these symptoms can manifest either during the transfusion process or in the 6-hour period after the transfusion. Typically, they occur within the first hour after transfusion [3]. In this case the patient showed hypotension and tachycardia. No cyanosis or fever was observed. The patient was on ventilator thus tachypnea is difficult to be assessed. Symptoms in this case were observed within 6 hours post-operatively without other risk factors for ALI.
Physical examination may reveal shallow breathing, diffuse crackles over the lung fields, and decreased breath sounds. Bilateral subtle infiltrates without cardiomegaly were evident on chest radiography, effectively excluding the possibility of cardiogenic edema. If pink, foamy secretions may be seen during intubation [1,9]. On physical examination, vesicular breath sounds were found, bilateral crackles without wheezing. Chest radiography showed bilateral subtle infiltrates without cardiomegaly. In our case, the patient showed similar symptoms, which are hypotension with blood pressure of 85-102/45-65 mmHg on the first day post-surgery, tachycardia and bilateral rhonchi breathe sounds. On X-ray examination, bilateral pulmonary infiltrates were found. Blood gas analysis also supported the picture of respiratory failure with SaO2 83%.
Hemodynamic monitoring can also be helpful in differentiating cardiogenic pulmonary edema and TRALI. Characterized by a pulmonary capillary wedge pressure within the normal or low range, TRALI necessitates hemodynamic monitoring for accurate diagnosis. This is crucial to differentiate it from other conditions with similar symptoms, including bacterial infections, cardiogenic pulmonary edema, anaphylactic reactions, or ARDS. Hypocomplementemia, leukopenia, neutropenia, and hypoalbuminemia may occur in some cases. Transient leukopenia, occurring in 5-35% of patients, stands out as the most common symptom [3]. In this case, hemodynamic, laboratory and AGD monitoring was carried out. Leukocytes were within normal limits, and albumin was slightly decreased. Complement was not examined in our case.
A prevalent feature of transfusion reactions is respiratory distress. It is imperative to exclude other types of transfusion reactions, such as TACO, transfusion-associated dyspnea (TAD), transfusion-associated bacterial sepsis, and severe allergic reactions [4,10,16]. Typically, TACO arises due to cardiogenic pulmonary edema caused by elevated hydrostatic pressure, which shows evidence of fluid overload before transfusion [8]. Exclusion of severe allergic transfusion reactions, such as anaphylaxis and urticaria, is also crucial in the diagnostic process. TRALI patients may exhibit symptoms like fever, hypotension, tachycardia, and cyanosis. However, it is important to note that wheezing and stridor, often linked with urticaria and allergic reactions, present clinically differently and do not induce pulmonary edema [10]. In this particular case, there were no observed instances of wheezing or stridor associated with urticaria or allergic reactions, ruling out the possibility of anaphylaxis. In this instance, the patient presented with low blood pressure, a normal temperature, and a chest X-ray devoid of vascular congestion or pleural effusion so it was more inclined towards TRALI than TACO.
Distinguishing between severe hemolytic reactions or transfusion-related sepsis and TRALI can be challenging, as both may manifest with hypotension and fever. In addition, tachypnea may occur due to an elevated systemic demand for oxygen. To differentiate TRALI from suspected sepsis and TAD, laboratory tests, such as culture and Gram stain of haptoglobin, LDH, urinalysis, bilirubin analysis, and blood products, can provide valuable insights. Patients could receive TAD diagnosis in the absence of any other identified cause for shortness of breath or tachypnea [10]. In this case the patient did not have any fever. Bilirubin examination was within normal limits, while examination for other infection markers was not evaluated.
Currently, supportive care remains the primary approach for treating TRALI, as no definitive treatments have been established. This care includes maintaining hemodynamics effectively through oxygen inhalation, ventilation, and extracorporeal membrane oxygenation [10]. Supportive modalities are such as 5% albumin, erythropoietin, and iron, in exceptional instances of sickle cell disease during TRALI incidents. Despite the common occurrence of pulmonary edema in TRALI, avoiding diuretics is advisable to prevent the potential hypotensive risks [17]. As a precaution, it is recommended to meticulously monitor fluid balance [10]. Effectively reducing barotrauma in patients on ventilators involves targeting lower peak pressures, thereby addressing risk factors for ALI. In this case, the patient received supportive therapy in the form of oxygen supplementation and installation of a PCV mode ventilator, PC 18 PEEP 12 FiO2 100% rate 26 Ti 0.95, flow trigger 2.0 with Ppeak 30, MV 9.2, TV 300-320, Ft 26.
The administration of high-dose ascorbic acid, a water-soluble vitamin, has been shown to limit damage caused by reactive oxygen species (ROS) to the epithelial barrier. High-dose ascorbic acid, administered intravenously, resulted in better 7-day survival for TRALI patients in critical condition, as demonstrated in a randomized controlled trial [18]. Steroids, although potentially beneficial in supporting spontaneous breathing and lowering mortality, lack substantial evidence to confirm their effectiveness in patients with TRALI, some ARDS studies have also reported reductions in systemic inflammatory markers. Controversy surrounds the role of steroids in TRALI treatment, and despite their use, the administration of steroids in numerous major studies did not result in improved clinical outcomes [10]. In this case the patient was given Dexamethasone 5 mg/8 hours although its function is still debatable.
The identification of both the donor and the immunoimmunized recipient is essential in cases of antibody-mediated TRALI. Donors necessitate testing for anti-HLA I, anti-HLA II, and anti-HNA antibodies. Flow cytometry with microbeads, enzyme immunoassay, lymphocyte immunofluorescence, lymphocytotoxicity, or other validated tests are employed for the antibodies detection to HLA class I antigens. To identify antibodies directed against HLA class II antigens, testing relies on enzyme immunoassays and flow cytometry with microbeads. It is recommended to utilize a combination of the Granulocyte Agglutination Test (GAT) and the Granulocyte Immunofluorescence Test (GIFT) for identifying HNA antibodies. An ideal approach involves conducting an antigen test on the recipient as well for a comprehensive assessment [10]. However, no antibody test was carried out in this case.
Implementing risk mitigation measures, involving the management of donors, processing of blood components, and the practice of patient blood management (PBM), has significantly reduced the morbidity linked to TRALI. Antibody-mediated TRALI prevention strategies include donor management and solvent/detergent-treated pooled plasma (SDP). To address the higher frequency of anti-HNA or anti-HLA antibodies in multiparous donors, risk reduction strategies for TRALI have been implemented. These include the adoption of male-dominated plasma, male-only donors, antibody screening, and exclusion of all-exposure donors. These measures have led to a substantial decrease in the morbidity linked to antibody-dependent TRALI in developed nations [19]. The manufacturing process of SDP involves treating large pools of plasma with solvent detergent to verify that levels of anti-leukocyte antibodies are beneath the detection threshold. In Norway, where SDP was adopted in 1993, no TRALI cases were documented within a 10-year timeframe. Until 2020, no TRALI cases had been reported in association with SDP transfusion [20]. Kumar et al.'s recent report suggests that regulatory T cells and IL-10 might have a preventive role in antibody-mediated TRALI. However, the IL-10 efficacy in preventing or treating TRALI in humans has yet to be conclusively determined.
Aspirin's ability to prevent TRALI in mouse trials by reducing lung platelet sequestration did not translate into a protective effect against TRALI in critically ill adult patients, according to a case-control study. As TRALI initiates, experimental studies indicate an increase in complement activation, including C3a and C5a, along with elevated levels of protein in bronchoalveolar lavage fluid and various chemokines, including IL-6 [2,10].
On the other hand, antibody-independent TRALI prevention strategies include TRALI patient blood management, platelet additive solution, pathogen reduction technology (PRT), and leukoreduction. The deliberate filtration of leukocytes in donated samples, known as leukoreduction, aims to lower the concentration of mediators produced by platelets and leukocytes. This process ultimately reduces the occurrence of adverse reactions associated with transfusion [21]. Proven to enhance the safety of blood components, pathogen reduction technology (PRT) specifically focuses on pathogen nucleic acid or membrane lipid structures in donor samples [22-25]. Preclinical studies have demonstrated inconsistent efficacy in utilizing pathogen reduction technology (PRT) to lower the risk of TRALI. Platelets donated by females, especially when stored in female plasma containing anti-HLA or anti-HNA antibodies, exhibited a markedly increased TRALI occurrence. Implementation of additional strategies, such as replacing traditional residual plasma with novel PAS in buffy coat pooled platelets, is crucial to further decrease the TRALI incidence [26]. Finally, patient blood management (PBM) seeks to enhance the patient's hematologic capacities, minimize bleeding, and curtail unnecessary transfusions as the ultimate objective [27]. Investigations into the potential benefits of other modifications to red blood cells (RBC) to mitigate the risk of TRALI are still ongoing [16].
TRALI mortality rates range from 5%-25%, but with good ventilator support, 80% of patients are reported to recover within 48-96 hours. TRALI confirmation can be performed when the anti-HLA or anti-HNA in the donor serum matches the patient's phenotype [7]. Individuals who have experienced TRALI exhibit long-term lung function comparable to those who have never encountered TRALI. Moreover, there are no additional complications, such as fibrosis or structural damage to the lung parenchyma, attributable to TRALI. Patients with TRALI may undergo a clinical course marked by the swift resolution (approximately two days) of hypoxemia. Immediate reporting of suspected TRALI cases to the blood bank is imperative. To identify donors with anti-HLA and anti-HNA antibodies and prevent their future donations, blood banks should thoroughly investigate all related donors associated with TRALI cases [8]. With adequate ventilator assistance, the patient slowly improved starting on the 4th day of treatment and was discharged on the 7th day.
Conclusion
TRALI manifests as non-cardiogenic pulmonary edema within a time frame of 6 hours post-blood product transfusion. Compared to other causes of acute respiratory distress syndrome, TRALI severity spans from mild to severe, with a minority of patients succumbing to the condition. Serious morbidity, including prolonged mechanical ventilation and extended stays in intensive care units and hospitals, is often encountered by many TRALI patients. In the case presented in this study, a 15-years-old male patient was reported who suffered TRALI after an intraoperative blood product transfusion during surgical resuscitation following a traffic accident for indications of grade 5 kidney rupture, survive with good supportive management of adequate oxygenation and ventilatory support.
Acknowledgments
We express our gratitude to the Department of Anesthesiology and Reanimation, Faculty of Medicine, Universitas Airlangga, and Dr. Soetomo Regional Public Hospital, Surabaya.
Funding
There was no specific funding from governmental, commercial, or non-profit entities for this study.
Authors’ Contributions
FMA and PM have made substantial contributions to the conception; design of the work; the acquisition, analysis, and interpretation of data; have drafted the work or substantively revised it.
Conflicts of Interest
The authors declared that there is no conflict of interest in this study
Consent to participate
The authors certify that they have obtained all appropriate patient consent forms. In the form, the parents have given their consent for images and other clinical information to be reported in the journal. The family understand that names and initials will not be published, and due efforts will be made to conceal identity, but anonymity cannot be guaranteed.
Ethical consideration
Not applicable.
Data Availability
The article contains all the necessary data to support the study; no supplementary source data is needed.
Orcid:
Faiz Muhammad Ammar*: https://orcid.org/0009-0001-2449-3028
Pesta Parulian Maurid Edwar: https://orcid.org/0009-0007-1324-1785
------------------------------------------------------------------------------------
How to cite this article: Faiz Muhammad Ammar, Pesta Parulian Maurid Edwar, Transfusion-related acute lung injury (TRALI) after surgical resuscitation in renal trauma patients: A case report. Journal of Medicinal and Pharmaceutical Chemistry Research, 2024, 6(9), 1403-1415. Link: https://jmpcr.samipubco.com/article_194467.html
------------------------------------------------------------------------------------
Copyright © 2024 by SPC (Sami Publishing Company) + is an open access article distributed under the Creative Commons Attribution License(CC BY) license (https://creativecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.

.png)
.png)
.png)
.png)
